Project Overview
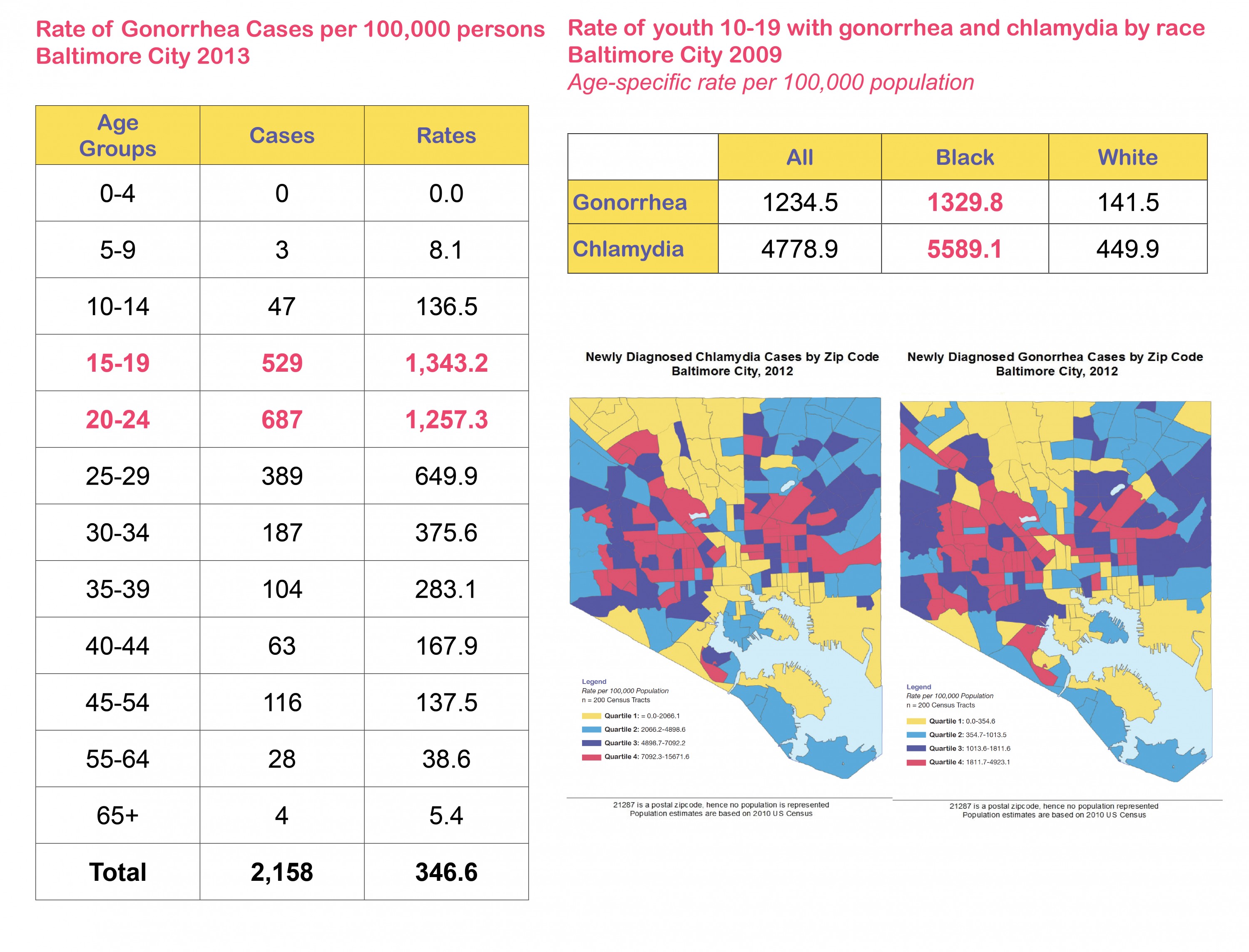
Baltimore has a long history of epidemic and endemic rates of sexually transmitted infections (STIs) and is a city with racial and ethnic disparities in STIs that are two to four times the national average. Young people in the U.S. represent 50% of all new STIs, while in 2012, young people in Baltimore represented 70% of new STIs reported to the Baltimore City Health Department (BCHD).
To address this issue, BCHD and the Johns Hopkins Center for Child and Community Health Research (CCHR), in collaboration with the Maryland Institute College of Art (MICA) Center for Social Design, received a three-year grant from the Centers for Disease Control and Prevention (CDC) in 2014 titled Community Approaches to Reducing STIs, or “CARS.”
To aid in the development of interventions to promote STI testing among young people in Baltimore, BCHD's Youth Advisory Council and partners collaborated with an interdisciplinary team of students at MICA’s Center for Social Design.
Together, they researched attitudes about STI testing among Baltimore youth, identified opportunities for intervention, and created youth-centered design solutions to improve the testing experience at local BCHD STI clinics and promote positive sexual health messaging through social media and in schools.
Research
The MICA team completed their own testing journeys, reviewed current literature, observed clinic spaces, interviewed, surveyed, and spent invaluable hours getting feedback from and workshopping ideas with Baltimore youth, clinicians, and health department staff.
Synthesis
Based on this research, the team identified six key design principles to help make the STI testing process a more positive experience for youth:
- Sex Positive: Youth need sexual health care experiences to move away from being punitive or judgmental and towards being supportive and positive.
- Comforting: Clinic spaces and testing can be “cold” and “scary” to a young person.
- Confidential: Youth and clinicians have different definitions of confidentiality. Clinicians follow HIPPA. Youth want to feel “invisible.”
- Timely: The longer youth have to wait, the less likely they’ll complete the testing process.
- Enjoyable: This is often the first time young patients are interacting with the clinic and STI testing— we want them to have a positive testing experience.
- Transparent: Youth want to know what the testing process will be like before they go.
The most important takeaway from the research was that ultimately, what is good for Baltimore youth is good for everyone.
Ideate
After synthesizing the research, the team identified two areas of opportunity for interventions:
- Improving the testing experience at a local BCHD STI clinic.
- Promoting positive sexual health messaging through social media and in schools.
Prototype
Additional conversations and ideation with youth and clinicians resulted in the following prototypes:
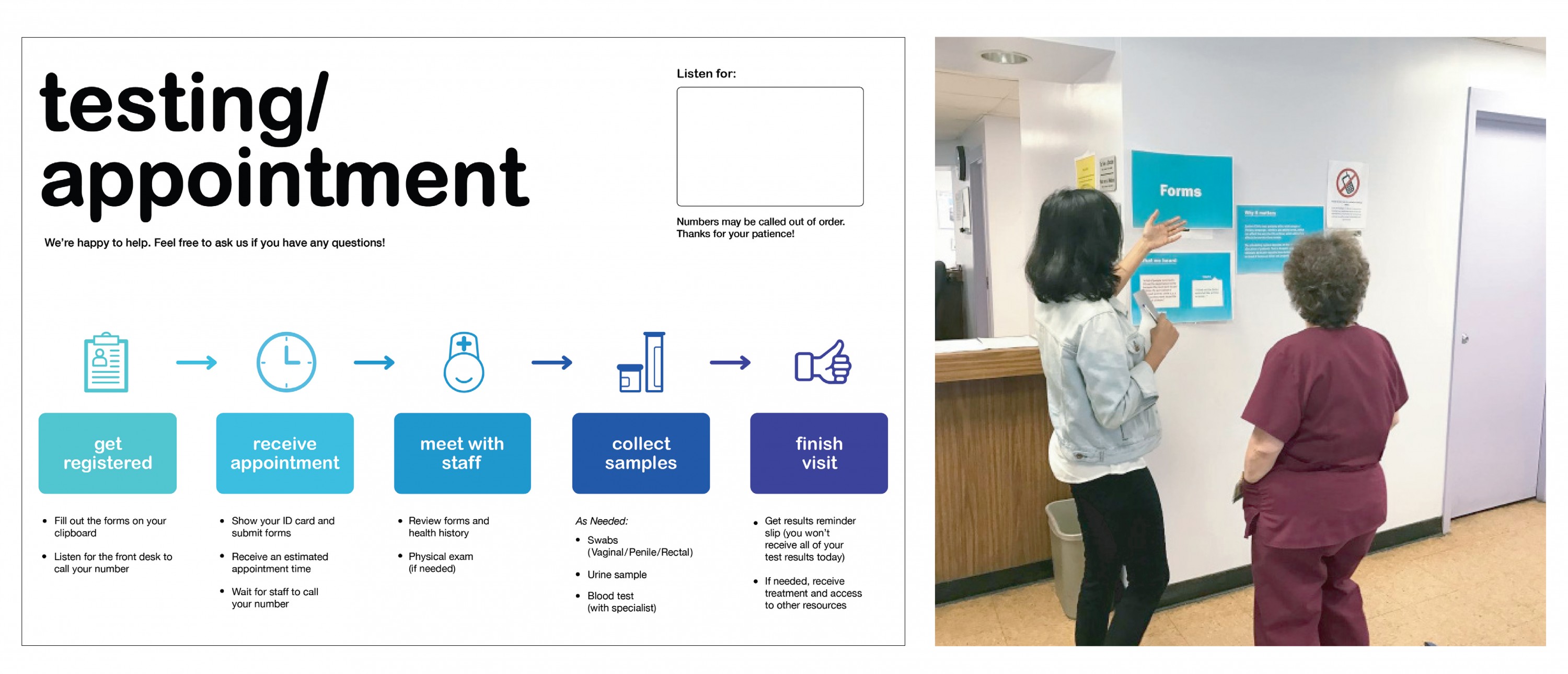
Testing Process Map: To help ease patient anxiety, the team worked with clinic staff at BCHD’s Eastern Clinic to develop a testing flow chart. The students then redesigned the clinic number system to include the testing process and placed the process graphic on key clinic walls.

Redesigned Forms: Eastern Clinic sees patients with a wide range of literacy, language, comfort, and ability levels, affecting the way they fill out forms, which affects the accuracy of their triage, and ultimately the service they receive. With input from clinic staff, the team redesigned the existing registration and triage forms to be easier to interpret. The goal of the new form is to (1) create a more positive registration experience for youth and (2) facilitate more a more accurate and efficient triage of patients.

Stay Sexy, Stay Healthy, Get Checked: The YAC and MICA team developed the "Stay Sexy, Stay Healthy, Get Checked" campaign. The campaign is visually bright and celebratory, uses youth-friendly messaging (“Sexual Health Check” vs. “STI Test”), and features quotes about sexual health from local youth.
Implement + Iterate
After implementing the new testing forms and process graphics, the team surveyed over 300 clients at Eastern Clinic to assess changes pre/post-intervention implementation. We found that post-intervention, clients were most likely to agree that they knew what to expect during their visit and that the form was easy to understand.
Articles & Publications
- Identifying Solutions to Improve the Sexually Transmitted Infections Testing Experience for Youth Through Participatory Ideation. S. Grieb, M. Reddy, B. Griffin, A. Marcell, S. Meade, B. Slogeris, K. Page, J. Jennings. AIDS Patient Care and STDs, Volume 32, Issue 8, 2018
- Stay Sexy, Stay Healthy, Get Checked: Designing a Youth-Friendly STI Testing Experience
- Youth Friendly Sexual Health Messaging Design Guide
- Youth Friendly Sexual Health Clinic Design Guide
- Ethics in Design and Communication: Critical Perspectives
Project Team
Sheldon Allen, Matthew Barr (MASD '17), Jayne Chartrand (MASD '17), Valeria Fuentes (MASD '18), Maria Garcia Diaz (MASD '17), Brittany Griffin, Devika Menon (MASD '17), Patricia Natalie (MASD '17), Molly Reddy (MASD '17), Rachel Serra (MASD ‘17), Irina Wong (MASD '17), Cynthia Zhu (GD MFA '17)
Project Partners
C. Patrick Chaulk, MD, MPH, Vira David-Rivera, Vanessa Geffrard, Suzanne Grieb, Ph.D., MSPH, Charlotte Hager, Jacky Jennings, Ph.D., MPH, Dr. Luke Johnsen, DO, Andy Masters, Sophie Meade, Glen Olthoff, Dr. Kathleen Page, MD, Tina Suliman, Paula Stauffer
Lead Faculty
Becky Slogeris
